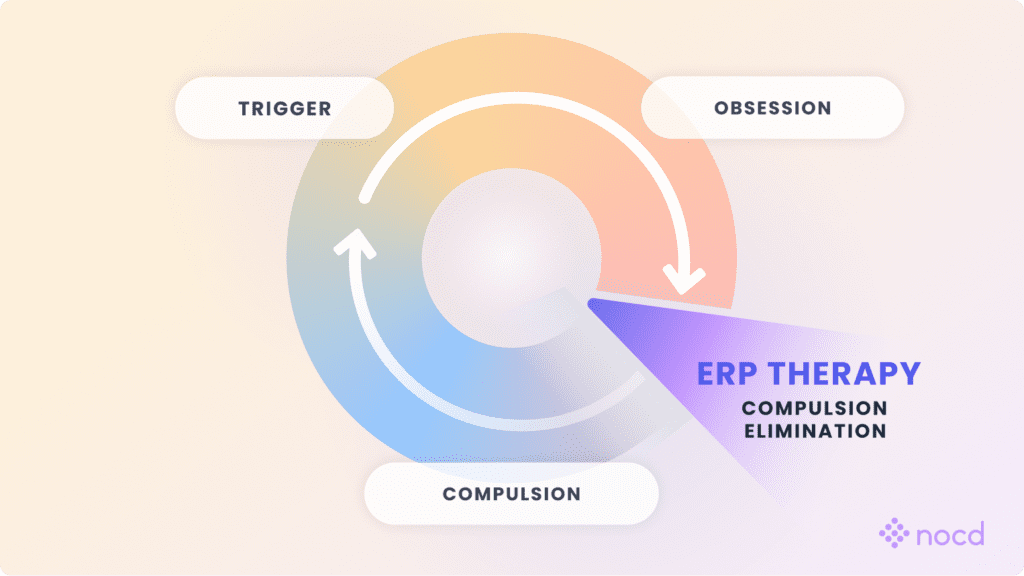
Exposure and response prevention (ERP) therapy is the first-line, evidence-based treatment for obsessive-compulsive disorder (OCD). It helps people break the cycle of obsessions and compulsions by gradually facing fears without performing rituals. Decades of research show ERP therapy is the most effective treatment for OCD, helping about 80% of people experience significant symptom relief.
Here’s a look into how ERP breaks the OCD cycle, why this form of therapy is so successful at treating OCD, and how you can get started with your own treatment.
What is ERP therapy?
ERP is a specialized form of cognitive behavioral therapy (CBT) proven to be effective for OCD. General CBT, if not tailored for OCD, can sometimes be unhelpful or even worsen symptoms. ERP helps people confront intrusive thoughts and anxiety while resisting the urge to perform compulsions.
“Exposure and response prevention is really the ‘B’ part of cognitive behavioral therapy,” says Patrick McGrath, PhD, Chief Clinical Officer at NOCD. “It very explicitly focuses on the behavioral aspects of OCD.”
The approach is endorsed by the American Psychiatric Association (APA), the National Institute for Health and Care Excellence (NICE), and the World Health Organization (WHO) as the first-line treatment for OCD.
How does ERP work?
ERP works by teaching people to tolerate anxiety and uncertainty instead of relying on compulsions.
It has two main parts:
- Exposure: Gradually facing thoughts, images, feelings, urges, sensations, or situations that trigger obsessions.
- Response prevention: Resisting the compulsive behaviors that usually follow.
Through repeated practice, the brain learns that anxiety naturally decreases over time—even without completing rituals. This process, known as habituation, breaks the cycle of OCD and helps people regain control of their lives.
ERP vs. other OCD treatments
ERP is more effective than talk therapy or medication alone, but it can be combined with other treatments.
- Talk therapy: Insight-oriented therapy has little impact on OCD symptoms compared to ERP.
- Medication: Selective serotonin reuptake inhibitors (SSRIs) can reduce OCD symptoms and are often used alongside ERP.
- Other therapies: Acceptance and commitment therapy (ACT) and mindfulness approaches can complement ERP, but don’t have the same level of evidence.
What happens in an ERP session?
In ERP therapy sessions, therapists guide people through structured steps:
- Assessment and education: Understanding the person’s OCD symptoms and explaining how ERP works.
- Exposure hierarchy: Creating a personalized list of ERP exercises, ranked from least to most distressing.
- Gradual exposures: Starting with easier triggers, the person practices facing fears while resisting compulsions.
- Homework: Practicing exposures in daily life between sessions.
A typical course lasts 12-20 sessions, but treatment length varies depending on symptom severity and progress.
ERP examples for different OCD subtypes
ERP treats all OCD subtypes, which are the subjects that your symptoms revolve around. Some examples of common OCD subtypes include harm, contamination, relationships, and perfectionism. Depending on how your OCD presents, you and your therapist will create ERP therapy exercises that are personalized to address your intrusive thoughts and compulsions.
Here are some examples of how ERP might look for different OCD subtypes:
| Obsession | Compulsion | Response prevention technique |
| What if I stab my partner with a kitchen knife? | Avoiding sharp objects | Handling sharp objects near others |
| I’m afraid that if someone who is sick touches me, I’ll get deathly ill. | Excessive handwashing and/or sanitizing | Deliberately touching “contaminated” surfaces without immediately washing hands or sanitizing |
| If the books on my shelf aren’t perfectly lined up, something bad will happen. | Repeatedly rearranging or aligning items until they feel “just right” | Purposely leaving books slightly askew or out of order without fixing them |
| What if my partner is not “the one?” | Seeking constant reassurance from your partner or others | Working with your partner to agree to no longer answer questions that have been asked and answered |
| What if I offend God by thinking about something sinful? | Excessive prayer and/or confession | Allowing sinful thoughts to be there without trying to neutralize them |
How effective is ERP for OCD?
ERP therapy is considered the most effective treatment for OCD.
Research consistently shows:
- Around 80% of people with OCD experience significant improvement after ERP.
- The benefits of ERP are long-lasting, especially when individuals continue to apply the skills after therapy.
- Relapse rates are lower compared to talk therapy or medication alone.
Real-world data also support ERP therapy. For example, NOCD’s teletherapy program found that members experience a 43% average reduction in OCD severity after 12 weeks of ERP therapy.
Who can benefit from ERP?
As mentioned, ERP is effective for all OCD subtypes, no matter how taboo. Research also supports the use of ERP for children, teens, and adults. Treatment is always adapted to each person’s symptoms and needs.
How to start ERP therapy
ERP should always be done with a trained OCD specialist.
Steps to get started include:
- Assessment: A mental health professional evaluates symptoms to confirm an OCD diagnosis.
- Finding a therapist: Look for providers who specialize in ERP, whether in-person or online. The IOCDF provider directory and the 650+ therapists in the NOCD Therapy directory are a good starting point for your search.
- Creating a plan: Work with your therapist to develop an exposure hierarchy.
- Beginning therapy: Start with smaller exposures and build up to more difficult ones over time.
Find the right OCD therapist for you
All our therapists are licensed and trained in exposure and response prevention therapy (ERP), the gold standard treatment for OCD.
Is ERP only used for OCD?
ERP is not just effective for OCD but for other mental health disorders, too. “Most anxiety-related disorders are treated with ERP, like panic disorder, social anxiety disorder, generalized anxiety disorder, or phobia,” says Tracie Ibrahim, LMFT, CST, Chief Compliance Officer at NOCD.
A specific type of ERP can also help manage post-traumatic stress disorder (PTSD). “There’s a variant of ERP called prolonged exposure that you can use for post-traumatic stress disorder,” adds Dr. McGrath. “There are numerous applications for exposure and response prevention therapy.”
FAQs about ERP
Is ERP therapy safe?
Yes. While ERP can feel uncomfortable at first, it’s done gradually and with support. Therapists ensure exposures are safe and manageable.
How long does ERP take to work?
Most people see improvement within 12–20 sessions, though results vary. Some notice relief in just a few weeks.
Does ERP work for intrusive thoughts for pure O?
Yes. ERP is effective for intrusive thought-based OCD as well as compulsions that are mental rather than physical.
What if ERP feels too hard?
ERP therapists adjust the pace to suit each individual. Treatment starts with smaller exposures and builds confidence before tackling more difficult triggers.
Bottom line
ERP therapy is the most effective OCD treatment across all subtypes and age groups. By facing fears without engaging in compulsions, people learn to tolerate anxiety and break the OCD cycle. With the guidance of a trained therapist, ERP helps individuals reduce symptoms, improve their functioning, and regain control over their lives.
Key takeaways
- ERP is the most effective treatment for OCD, supported by decades of scientific research.
- It works by exposing people to their fears (exposure) while resisting compulsions (response prevention).
- ERP is effective for all OCD subtypes and across age groups.
- Most people see improvement within 12–20 sessions, especially when guided by a trained OCD specialist.