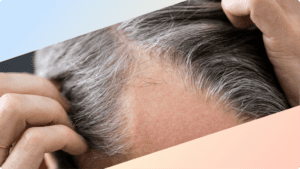
It’s not uncommon to pick at your skin. Most people pick their nose, and many pick at cuticles, scabs, or pimples. It can feel satisfying to pick, and the behavior is not always indicative of a larger problem.
However, excessive picking can be a sign of dermatillomania, or skin picking disorder—a mental health condition characterized by an irresistible urge to pick at your own body. If you’re worried about how often you’re picking, or the damage you’re causing, it can be helpful to better understand the features that define skin picking disorder, as well as potential triggers for the behavior. Read on to gain clarity about whether your skin picking is cause for concern, and how to find effective treatment.
What is skin picking disorder?
Skin picking disorder (also known as excoriation disorder or dermatillomania) is a type of body-focused repetitive behavior (BFRB) where you compulsively pick at your skin or scalp. A BFRB describes a repeated behavior performed on your body, such as biting your nails, pulling out your hair, or biting the inside of your cheek, lips or tongue. BFRBs can also coincide with other mental health conditions, including anxiety, depression, obsessive-compulsive disorder (OCD), attention-deficit hyperactive disorder (ADHD), and autism.
While it can be common to pick at small imperfections on your scalp, if your picking is leading to frequent bleeding and scabs (which you also pick off), you may be dealing with more than a bad habit. Skin picking disorder is usually difficult to stop on your own, and can cause significant distress—impeding your ability to go about daily life.
Impacts of scalp picking
If left untreated, skin picking and scalp picking can cause physical health issues. “Picking behavior can be responsible for serious skin infections,” says Nicholas Farrell, PhD, a licensed clinical therapist and Regional Clinical Director at NOCD. “Some people with untreated and severe excoriation disorder have actually required hospitalization.”
In addition to tissue damage and scarring, people with skin picking disorder often report feeling emotional distress, shame, blame, and low self-esteem. You might find that you avoid socializing because you’re worried that your habit will raise questions. Perhaps you even try to leave social situations in order to find a private place to pick, when the urge becomes too intense. Dr. Farrell says skin picking can become a significant distraction, impairing your ability to focus on tasks you need to accomplish.
Why am I picking my scalp?
If you’re picking your scalp regularly, causing damage, or struggling to stop, it’s worth learning more about skin picking disorder and BFRBs.
Understanding BFRBs
Scalp picking is a type of body-focused repetitive behavior (BFRB). While some people engage in BFRBs knowingly—but struggle to stop—it’s also possible to pick your skin repetitively without being aware of doing so. It may be such an ingrained habit you don’t even realize that your fingers are floating up toward your head to pick, until you start digging your nails in and scratching. At that point, it can feel difficult to reverse course.
Some people engage in BFRBs out of boredom, or to soothe feelings of anxiety, sadness or impatience. “Picking might offer relief from some kind of unwanted state, such as tension or stress,” Dr. Farrell explains. “Other people say that it fills a void in response to boredom or lack of sensory stimulation. In that case, picking is providing some sense of gratification or stimulation.” While picking your scalp can feel good in the moment, the long-term effects can be detrimental.
Understanding OCD compulsions
BFRBs like scalp picking often occur in people with OCD, but these are two distinct diagnoses. OCD is a complex mental health condition characterized by intrusive thoughts, feelings, urges, sensations, and images (known as obsessions) that can cause intense feelings of distress and anxiety. In response to these feelings, people with OCD engage in compulsions—repetitive behaviors or mental rituals meant to ease the discomfort brought on by their obsessions. For example, someone who experiences intrusive thoughts about their pet dying might react by constantly checking on their pet to make sure they’re breathing.
Like BFRBs, OCD compulsions are often performed in an attempt to soothe negative feelings. But, the reasons for engaging in these behaviors come from different places. People with BFRBs may be responding to discomfort, but aren’t typically reacting to specific intrusive thoughts. OCD compulsions, on the other hand, are performed in response to an obsession. Scalp picking is more likely to be a BFRB than an OCD compulsion, even though it can occur in people who are also navigating OCD.
It’s important to understand the differences between OCD compulsions and BFRBs because the treatments for each are different. While OCD is most effectively treated with exposure and response prevention (ERP) therapy—which slowly exposes you to your fears in an effort to build resilience—BFRBs are best addressed through habit reversal training (HRT) and comprehensive behavioral model (ComB). HRT and ComB focus on investigating what causes your scalp picking and developing alternative, healthier responses.
How can I stop picking my scalp?
As much as you try to stop, it may be challenging to give up scalp picking on your own. Seeking support from a therapist trained in BFRBs can be a crucial step toward regaining control.
Habit Reversal Training (HRT) for BFRBs
With BFRBs, including picking at your scalp, Dr. Farrell says the best treatment is habit-reversal training (HRT). HRT is a type of cognitive behavioral therapy that consists of two foundational elements:
- Awareness training
- Competing response training
Awareness training is the first step of HRT. It focuses on helping you learn what triggers your skin picking. With the guidance of your therapist, and a plan specialized to you and your unique needs, you’ll learn how to self-monitor and pay close attention to the feelings or situations that seem to cause you to pick your scalp. “Awareness training helps a [person] improve their identification and recognition of the warning signs…for skin picking,” says Dr. Farrell.
After you’ve worked on awareness training, you’ll learn about competing response training. This entails learning a behavior or response that can “compete” with the behavior that you want to stop—in this case, scalp picking. Dr. Farrell provides an example: “If you’re trying to prevent yourself from picking your scalp, you might fold your hands together in a clasp, which physically prevents you.” Other competing responses might include reaching for a fidget spinner, or knitting.
By developing a competing response, you put space between the urge to pick and the action to do so—giving you a chance to regain control over your behavior. “People are so quick to respond to that urge to pick, there’s never an opportunity to learn that even though it’s bothersome, you can endure the situation without giving into that craving,” Dr. Farrell explains. Resisting the urge one time won’t “cure” the condition, but by practicing these strategies, you can eventually ease the behavior. “The tolerance in one’s ability to accept and live with the urge grows and the intensity of that craving diminishes,” Dr. Farrell says.
While HRT can be highly effective for BFRBs, it does not address other potential underlying mental health conditions or emotional issues. It can be important to talk to your therapist about other strategies that may be needed. For example, if you also have OCD or anxiety, you may want to speak to your clinician about a combination treatment of HRT and exposure and response prevention (ERP) therapy—which is effective for both OCD and anxiety.
CTA: Find the right OCD therapist for you [therapist directory]
Comprehensive Behavioral Intervention (ComB) for BFRBs
The comprehensive behavioral model (ComB) is another treatment method that can be effective for BFRBs. ComB utilizes a more individualized approach, by spending more time focusing on the underlying factors that may be causing you to pick your scalp. Like HRT, ComB eventually utilizes methods for determining triggering feelings, activities or environments, so you can learn to turn to alternative behaviors during these moments.
Find the right OCD therapist for you
All our therapists are licensed and trained in exposure and response prevention therapy (ERP), the gold standard treatment for OCD.
Bottom Line
It’s not entirely uncommon to pick at your skin, but if picking your scalp is causing physical damage and impairing your ability to engage in daily life, it’s important to consider whether you may be engaging in a BFRB. If you’re feeling shame or physical discomfort as a result of your behavior, know that you’re not alone, and that it’s possible to find relief. Regardless of what triggers your scalp picking, therapists trained in treating BFRBs can help. You don’t have to carry this burden alone.
Key Takeaways
- Picking at your scalp can cause bleeding, infections, and impact daily life. You may find yourself struggling to focus, or avoiding social activities as a result of this behavior.
- While skin picking can occur alongside OCD, anxiety, and other mental health conditions, it is its own diagnosis.
- Seeking support from a therapist trained in treating BFRBs can be an important step in learning to stop picking.
- HRT and ComB are the most effective treatments for scalp picking. These forms of therapy can help you identify triggers and replace the behavior with healthier habits.