Harm OCD is a subtype of obsessive-compulsive disorder (OCD) that causes intrusive fears about harming yourself or others—even though you have no desire or intent to do so. These thoughts are distressing, unwanted, and often go against your values.
People with harm OCD might avoid knives, driving, or even holding loved ones because they’re terrified of losing control. But these fears don’t reflect intent or danger—they’re symptoms of OCD.
Harm OCD is very common, with research showing that 31.8% of people report experiencing harm-related obsessions.
What is harm OCD?
Harm OCD involves intrusive, repetitive thoughts, images, urges, feelings, or sensations about violence, accidents, or injury, paired with intense anxiety and compulsions to “prevent” harm.
This subtype can manifest in several forms:
- Self-harm OCD: Fear of intentionally hurting yourself.
- Hit-and-run OCD: Fear of accidentally harming someone while driving.
- Postpartum or perinatal OCD: Fear of hurting your baby or child.
- Suicidal OCD: Fear of acting on suicidal thoughts, despite not wanting to die.
All of these themes share the same core: intrusive thoughts about harm, misinterpreted as danger or moral failure.
If you ever feel you might act on suicidal thoughts or are in crisis, contact the 988 Suicide and Crisis Lifeline by calling or texting 988 (U.S. only). If you’re outside the U.S., you can find international hotlines here or visit your nearest emergency department.
What’s the difference between harm OCD and self-harm thoughts?
Harm OCD involves intrusive fears about harm, while self-harm thoughts usually stem from emotional distress or a desire to cope, not fear.
Here’s how the two experiences differ:
| Feature | Harm OCD | Self-harm thoughts |
| Core emotion | Fear, guilt, anxiety | Sadness, hopelessness, emotional pain |
| Intent | No intent to harm; thoughts are unwanted | Desire to relieve emotional pain |
| Thought pattern | Intrusive, repetitive, ego-dystonic | Reflects coping or self-punishment |
| Goal of behavior | Avoid or neutralize the thought | Regain control or express distress |
| Treatment approach | Exposure and response prevention (ERP) therapy | Emotion regulation and safety planning |
While the content may sound similar, the underlying mechanisms are very different. Someone with harm OCD may worry about hurting themselves, whereas someone experiencing suicidal ideation may feel they want to.
Is harm OCD dangerous?
No. Harm OCD is not dangerous, but it can be extremely upsetting or even debilitating for those who have it, due to the intense anxiety and fear.
The distress from this OCD subtype comes from a fear of losing control, not from violent urges. These thoughts often trigger guilt, shame, and confusion because they clash with the person’s actual values.
People with harm OCD may fear:
- Accidentally harming others (e.g., pushing someone off a ledge).
- Intentionally hurting loved ones.
- Losing control while driving.
- Self-harming without meaning to.
Avoidance behaviors—like hiding sharp objects or avoiding babies—are attempts to feel safe, but they only reinforce OCD’s cycle of fear and reassurance-seeking.
What are the symptoms of harm OCD?
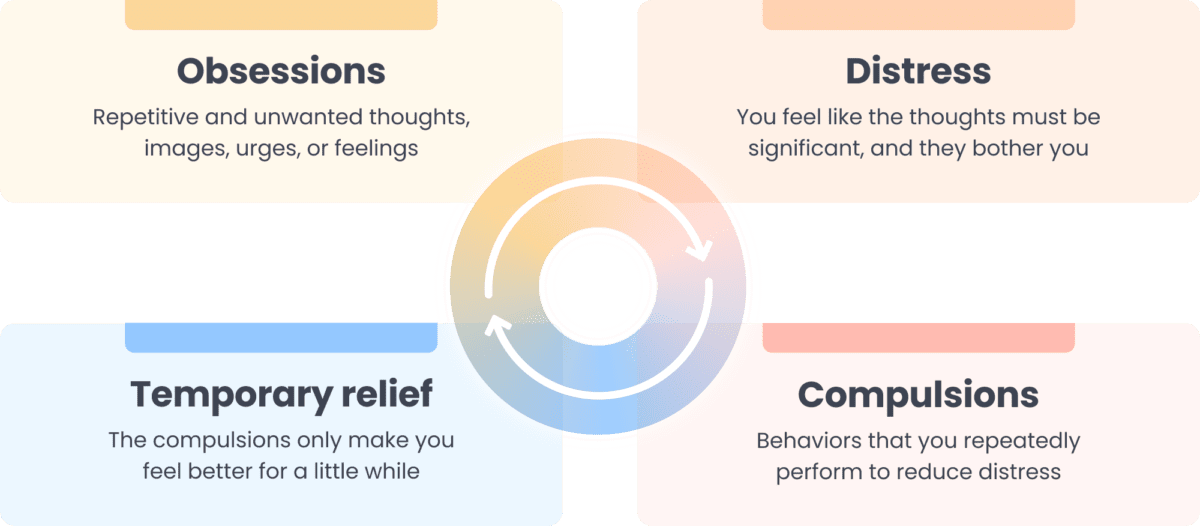
Harm OCD involves two symptoms: obsessions (intrusive thoughts, images, urges, feelings, and sensations) and compulsions (physical or mental acts done to relieve distress from obsessions or to prevent a feared outcome).
Harm OCD obsessions
- Thoughts or images of stabbing, hitting, or killing someone.
- Fear of losing control and hurting yourself.
- Mental images of violent or gory scenes.
- Fear you might suddenly swerve your car into traffic.
- Worry that you’ve already harmed someone and forgotten about it.
Harm OCD compulsions
- Avoiding triggers like knives, driving, or watching violent media.
- Seeking reassurance from others (“I’d never do that, right?”).
- Mentally reviewing past actions for proof that you didn’t harm someone.
- Praying, counting, or repeating phrases to “cancel” bad thoughts.
- Checking for signs of injury or evidence of wrongdoing.
What causes harm OCD?
There’s no single cause of harm OCD or any OCD subtype. OCD develops from a mix of genetic, biological, and environmental factors that affect how the brain processes uncertainty and threat.
Intrusive thoughts are common—more than 90% of people experience them—but in OCD, the brain misinterprets them as meaningful or dangerous.
What triggers harm OCD thoughts?
Harm OCD can be triggered by everyday stressors, media exposure, or situations involving responsibility or moral themes.
Common triggers include:
- Reading about violence or crime.
- Stressful life events or major transitions.
- Exposure to sharp objects, driving, or caring for others.
- Fatigue, anxiety, or emotional distress.
- Consuming violent or graphic content.
Triggers themselves don’t cause OCD—they activate existing fears and reinforce compulsive responses.
How is harm OCD diagnosed?
Harm OCD isn’t a separate diagnosis in the DSM-5. It’s recognized as a presentation of OCD. Diagnosis is typically made by a licensed clinician—preferably an OCD specialist—who evaluates:
- The presence of intrusive, unwanted thoughts about harm.
- Compulsive behaviors or avoidance linked to those fears.
- Distress or impairment in daily functioning.
If you’re unsure whether your thoughts are OCD-related, a specialist can help clarify and provide an evidence-based treatment plan.
When to seek help
Consider seeking professional help if:
- Intrusive harm thoughts are frequent or distressing.
- You avoid certain objects, people, or situations to feel “safe.”
- You spend excessive time checking, reviewing, or seeking reassurance.
- You feel unable to control your thoughts despite knowing they’re irrational.
- You experience guilt, shame, or anxiety that interferes with work, school, or relationships.
Early intervention with OCD-trained providers can make recovery faster and more sustainable.
How is harm OCD treated?
Harm OCD is manageable with several evidence-based treatments that can help break the cycle of intrusive fears and reassurance-seeking.
Exposure and response prevention (ERP) therapy for harm OCD
The most effective treatment for OCD is exposure and response prevention (ERP) therapy. ERP is a specialized form of cognitive behavioral therapy (CBT) proven to be effective for OCD. General CBT, if not tailored for OCD, can sometimes be unhelpful or even worsen symptoms.
ERP therapy helps you confront intrusive thoughts while resisting compulsions. Over time, this reduces anxiety and breaks the cycle of fear.
Examples of ERP exposures for harm OCD include:
- Holding a kitchen knife while cooking.
- Writing or saying feared phrases aloud (“I might hurt someone”).
- Driving past a location without checking for accidents.
- Watching mildly violent TV scenes without reassurance.
- Holding your baby or loved one under supervision.
Studies show that ERP therapy is highly effective, with 80% of people with OCD experiencing a significant reduction in their symptoms.
Find the right OCD therapist for you
All our therapists are licensed and trained in exposure and response prevention therapy (ERP), the gold standard treatment for OCD.
Supportive treatments
Medication (such as SSRIs) can help reduce obsessive thoughts and anxiety. Mindfulness-based strategies, acceptance and commitment therapy (ACT), and support groups can also improve resilience during ERP.
Treatments for severe or treatment-resistant harm OCD
Severe or treatment-resistant harm OCD may benefit from the following therapies:
- Intensive outpatient programs (IOPs)
- Partial hospital programs (PHPs)
- Residential treatment centers (RTCs)
- Transcranial magnetic stimulation (TMS)
- Deep brain stimulation (DBS)
- Gamma knife radiosurgery (GKRS)
FAQs about harm OCD
No. Violent thoughts are often intentional or linked to anger, while harm OCD thoughts are unwanted, fear-based, and distressing.
No. Harm OCD doesn’t compel people to act on their thoughts. The fear of doing harm is what causes distress—not any actual desire to do it.
Yes. With ERP therapy and consistent support, most people experience major symptom reduction. While intrusive thoughts may still appear occasionally, they lose power over time.
Intrusive thoughts are a normal part of human cognition. In OCD, the brain misfires—interpreting these harmless mental events as signs of danger or moral failure.
Bottom line
Harm OCD can be terrifying, but it’s not dangerous—and it’s treatable. Intrusive harm thoughts don’t define who you are or what you’re capable of.
With ERP therapy, professional support, and education, you can learn to accept uncertainty and stop letting OCD dictate your life.
Key takeaways
- Harm OCD is a common subtype of OCD where intrusive thoughts focus on causing harm to yourself or others, but these thoughts do not reflect your true intentions.
- Having harm-related thoughts does not make you dangerous—people with harm OCD are actually less likely to act on these thoughts.
- Effective treatments are available, including exposure and response prevention (ERP) therapy, ACT, medication, and other supportive approaches tailored to your needs.

