Dr. Carolyn Rodriguez is a foremost expert on obsessive-compulsive disorder (OCD) and conducts cutting-edge research aimed at improving our understanding of the brain and suggesting new treatment possibilities for people around the world.
She is Assistant Professor of Psychiatry and Behavioral Sciences at Stanford University, Member of the Stanford Neurosciences Institute, and Director of the Rodriguez Lab, which translates neuroscientific discoveries into new therapies.

This interview was conducted over the phone in late May 2018.
Patrick at NOCD: Thanks very much for speaking with us today, Dr. Rodriguez. Let’s start at the beginning. How did you get involved in researching OCD? Can you tell us a bit of your story?
Dr. Rodriguez: My interest in mental health started at an early age. I saw firsthand the impact of mental illness in my extended family, and I became interested in how differences in our brains can shape differences in our behavior. I trained to be a psychiatrist and neuroscientist and seek improved treatments for mental illness.
Early in my career, I met someone with OCD. I was immediately struck not only by his private suffering, but also by all of the physical manifestations that made his life harder. His distressing intrusive thoughts about contamination caused him to always wear gloves when he went outside. He washed his hands excessively. When he took his hands out of his gloves, they were red and raw. His pain made a big impression on me.

I became curious about what might be driving these behaviors. I wondered how an obsession forms, and how it transitions into a disorder. We all have out-of-the-blue intrusive thoughts like “Did I leave the stove on?” And we all have felt compelled to go back and check the stove.
But where along the way do these types of thoughts and behaviors cross a line, becoming the condition we know as OCD? The diagnostic standard is that intrusive thoughts and repetitive behaviors that occupy more than 1 hour a day, cause distress, and interfere with daily functioning cross that line. As I treated more individuals with OCD, I became very frustrated by our current first-line treatments. Medications like serotonin reuptake inhibitors and cognitive behavior therapy using exposure and response prevention (EX/RP or ERP) leave many individuals with residual symptoms.
There is also often a lag time of 2-3 months before substantial symptom relief is achieved. We urgently need more effective and faster-acting treatments for OCD. The mission of our lab is to innovate targeted, rapid-acting treatments and derive insights into the brain basis of OCD and related disorders in order to relieve patients’ suffering. We collaborate across disciplines to accelerate the discovery of treatments.
NOCD: How, specifically, does understanding the underlying brain mechanisms allow you to help people who are living with these conditions?
Dr. Rodriguez: We don’t know what causes OCD. But we increasingly think of mental illnesses as the result of brain circuits gone awry. OCD symptoms are associated with hyperactivity in the thought control circuit, which is comprised of the orbitofrontal cortex (important for decision-making), the striatum (motor movement), and the thalamus (a relay station back to the cortex). The hyperactivity may be due to imbalances of chemical messengers, called neurotransmitters, like serotonin and glutamate.
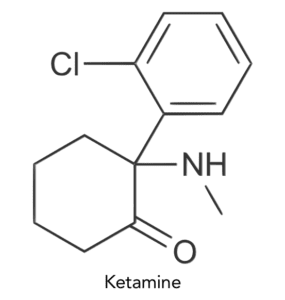
Increasing evidence indicates that glutamate plays a role in OCD symptoms. Ketamine– which at high doses is used primarily as an anesthetic– acts on brain receptors for glutamate, and has shown remarkable therapeutic effects in depression and other disorders. I led the first randomized proof-of-concept clinical trial comparing low-dose intravenous ketamine with placebo in fifteen OCD patients suffering from constant obsessions.
After a single ketamine infusion, half the patients met the response criterion (35 percent or greater reduction in the Yale-Brown Obsessive Compulsive Scale, or Y-BOCS, one week after infusion). The effect was rapid (within hours), and patients reported remarkable benefit. The effects persisted long past the half-life of ketamine, suggesting that beneficial effects remained long after ketamine had been cleared from the body. In some but not all individuals, the therapeutic effects persisted for two to four weeks.
Although these results are promising, patients did report side effects, including transient dissociation– a temporary experience of detachment from reality. Also, ketamine is a street drug of abuse, often called “Special K.” Because of ketamine’s substance abuse potential, in all our studies, we carefully screen and exclude individuals who may be at risk for addiction.

NOCD: Speaking of response to these novel treatments, I’ve always wondered if reducing the intensity of obsessions would automatically lead to a decrease in compulsions, or if those behaviors can somehow stick around, like a habit.
Dr. Rodriguez: What we heard from patients who benefitted from ketamine was interesting. They reported that even though their obsessive thoughts went away, they still had an inclination to check. Like you, we are curious how obsessions influence compulsions, and we wonder how we can pull apart and understand these differences.
Our lab next seeks to understand the mechanism underlying ketamine’s rapid therapeutic effects. We are conducting a large, randomized NIMH-funded study to examine how ketamine acts on the building blocks of brain function: the receptor, the circuit, and the circuit network. If you or a loved one have OCD and live in the San Francisco Bay Area, you can contact us at ocdresearch@stanford.edu to see if you are eligible to participate in this ketamine study, or other ongoing studies.
NOCD: It’s great to know about these really interesting pharmacological discoveries. It makes me wonder, though, how can medication and therapy can work together for someone who is trying to get better.
Dr. Rodriguez: I believe in the benefits of combining medication and cognitive-behavioral therapy– specifically ERP. Sometimes, starting therapy is hard; but medication may help decrease OCD severity enough to allow psychotherapy to begin. This may be an avenue for the use of a single dose of rapid-acting ketamine. If you break your arm, you may need pain medication to help you feel a bit better while your bone heals in a cast. Similarly, ketamine may make entry into therapy more tolerable. Ketamine may also work synergistically with therapy, given its role in learning and memory.
At the same time, ketamine’s effects do not appear to be long-lasting. Our team wondered: could we extend ketamine’s effects by combining it with a brief course of cognitive-behavioral therapy? Our rationale drew from two lines of research: previous studies suggesting ketamine may enhance brain plasticity and extinction learning in animal models, and trials that combined therapy with medications thought to facilitate extinction learning, reporting increased cognitive-behavioral therapy gains.
Our pilot study in ten adults with OCD gave a single intravenous ketamine dose followed by an abbreviated course of ERP (ten one-hour exposure sessions) delivered during the time when ketamine is thought to facilitate extinction learning (two weeks). We found that over 60% of subjects with OCD met the response criterion (35 percent or greater reduction in Y-BOCS score) at two weeks after the single ketamine infusion.

NOCD: Clearly there’s a lot of buzz right now around drugs– like ketamine, psilocybin, and LSD– that are typically thought of as dangerous or taboo. They’re also controlled substances in many countries, including the United States. Do you think it’s important to address these concerns as part of the research process?
Dr. Rodriguez: I do think it is important to address these points as part of the research process. Although our ketamine results are promising, patients did report side effects, as I mentioned. Additionally, enthusiasm must be tempered by what we don’t know. No large-scale studies of the risk of ketamine abuse or its safety with long-term administration have been conducted.
To find rapidly acting treatments without ketamine’s dissociative and other side effects, my lab is working to identify new compounds that act on the glutamate pathway. Rapastinel, an NMDA glutamate receptor modulator, has rapid antidepressant activity and minimal risk of ketamine-like side effects. It is currently in a large phase III research program that may identify it as a first-in-class FDA-approved treatment for depression.
Does rapastinel have similar effects in OCD patients? I led a team conducting an open-label, proof-of-concept study (n=7). We found that rapastinel (as a 10 mg/kg intravenous dose) decreased symptoms of OCD, anxiety, and depression within hours, and was well-tolerated. Rapastinel did not produce the dissociative or other side effects seen with ketamine administration. The effects of a single rapastinel dose on OCD symptoms did not, however, persist at one week post-infusion. So a next step for developing rapastinel in OCD is to try repeated dosing.

NOCD: So is there something that might be paired with ketamine on a medication front to give longer-term relief?
Dr. Rodriguez: Yes, we are conducting research studies to explore how we can best treat individuals. One study utilizes transcranial magnetic stimulation (TMS). We are focused on how to rapidly help individuals with OCD symptoms, and because current treatments with TMS take months, we would love to be able to create more rapid effects in OCD. One of the advantages of TMS is that it doesn’t have the systemic side effects that many drugs have. And it can be targeted to the brain area that contains the thought control circuit. We’re thinking about a wide range of treatment strategies– medication, therapy, non-invasive brain stimulation– and how we can use the synergy of these different kinds of treatments to make a real impact on patients’ symptoms.
If you or a loved one have OCD and live in the San Francisco Bay Area, you can contact us at ocdresearch@stanford.edu to see if you are be eligible to participate in this TMS study.

NOCD: We’ve definitely been hearing more about TMS lately, and it’ll be exciting to see further studies emerge. More generally, what might you tell someone who’s intimidated by the idea of participating in a clinical trial?
Dr. Rodriguez: I would say you are not alone. Deciding to participate in a study would make anyone anxious. But to feel more comfortable with study participation, you can start by educating yourself. Here are three questions you can ask:
1) Does the science behind the study interest you? There is a scientific rationale for every research study. Each study is seeking to find the answer to a specific question and advance the field. Is that question clear to you? Are you curious about the answer? Knowing exactly how and why you can contribute to OCD research might be motivating (and inspiring).
2) Do you know what the particular study entails– and do you have the time to participate?
Every study is different, and they require different levels of involvement. Some studies involve several visits over the course of months; others require one visit. Some request a blood sample; others involve neuroimaging; still others involve ongoing treatment. Make sure you are informed about the timing and the content of the study procedures so that you can decide whether or not you have the necessary time and interest.
3) Do you want to work with the research team?
Follow-up questions include: Do they have a good track-record of publishing results? Do they have funding from the National Institutes of Health or other peer-reviewed agencies? Do they seem responsive, kind, and knowledgeable? Are they informing you of your rights as a study participant? Do they explain that your participation is voluntary? Do you know who you can contact if any issues come up?
Participating in a research study is a very selfless, altruistic act. I am incredibly thankful to each one of our study participants, who are improving our understanding of OCD for the entire OCD community. Wherever you live, you can find out more about research studies in your area by visiting clinicaltrials.gov.

NOCD: These are great questions to think about. But we do get some frustration in our community, with people asking why there hasn’t been a new medication option for OCD since 1997. Researchers were talking about glutamate quite a while ago, for example, so why is it taking so long to have new possibilities?
Dr. Rodriguez: I share that frustration. It has lit a fire in me, but I think we are closer than ever. Rapastinel is in phase 3 studies for major depression, and may be approved by the FDA as early as 2021. Our small pilot study that I mentioned earlier will help providers make a case for insurance reimbursement for OCD.
We are also a study location for a phase II clinical trial comparing the efficacy of a glutamate modulator called trigriluzole (BHV-4157) versus placebo in OCD, sponsored by Biohaven Pharmaceuticals.
NOCD: That’s great to hear– seems like there’s a lot of research happening right now. Is there anything else you’d like to say today?
Dr. Rodriguez: I am very hopeful about our ongoing research studies, which are identifying new pathways for novel treatments. We are looking forward to not only partnering with people who want to participate in our clinical studies, but also to partnering with nOCD and other organizations like the International OCD Foundation (iocdf.org) and the Anxiety and Depression Association of America (adaa.org) to raise awareness about OCD treatments and research studies. I see so many people suffering in silence. We are active in the community, co-sponsoring a free OCD awareness day here at Stanford, raising money for the IOCDF each year through the 1 Million Steps 4 OCD walk, and writing articles to connect patients to existing treatment options– and to novel research for those not helped by standard treatments.
I am very humbled and inspired by those who are willing to participate in a research study. We approach treatment development from the science and research sides, but we need partners who are experts in their own symptoms in order to understand if these treatments work. Because of HIPAA and confidentiality, I cannot publicly thank individuals who have donated their time, but I am very thankful for their participation.
NOCD: Thanks very much for your time, Dr. Rodriguez. A number of us have OCD, and we’re really excited about this research. We’re grateful to you and your team for all your hard work.
Click here to get more information about current studies at the Rodriguez Lab.
For the latest news, follow Dr. Rodriguez (@CRodriguezMDPhD) and Rodriguez Lab (@RodriguezLabSU) on Twitter.
If you or someone you know is struggling with OCD, schedule a free call today with the NOCD clinical team to learn more about how a licensed therapist can help. ERP is most effective when the therapist conducting the treatment has experience with OCD and training in ERP. At NOCD, all therapists specialize in OCD and receive ERP-specific training.

